Join Opencare to
get profitable patients
grow the easy way
save your team time
Opencare sends you ready-to-book patients who are matched to your practice for long term fit. And you only pay after successful patient visits.
2,500+

30+

400,000+

4.8

Trusted by top dentists
Receive high-need patients who are ready to book
Only pay for successful patient visits — no lead fees
No disruption to your workflows — more time for your patients
Explore for yourself, in our interactive platform tour
How it works

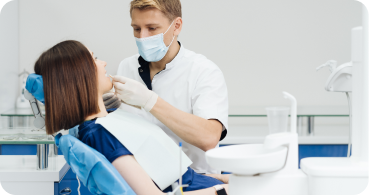
Ready-to-book patients complete a survey
They share treatment needs, insurance, and preferences – so we can match them with the best dentist for long-term fit.

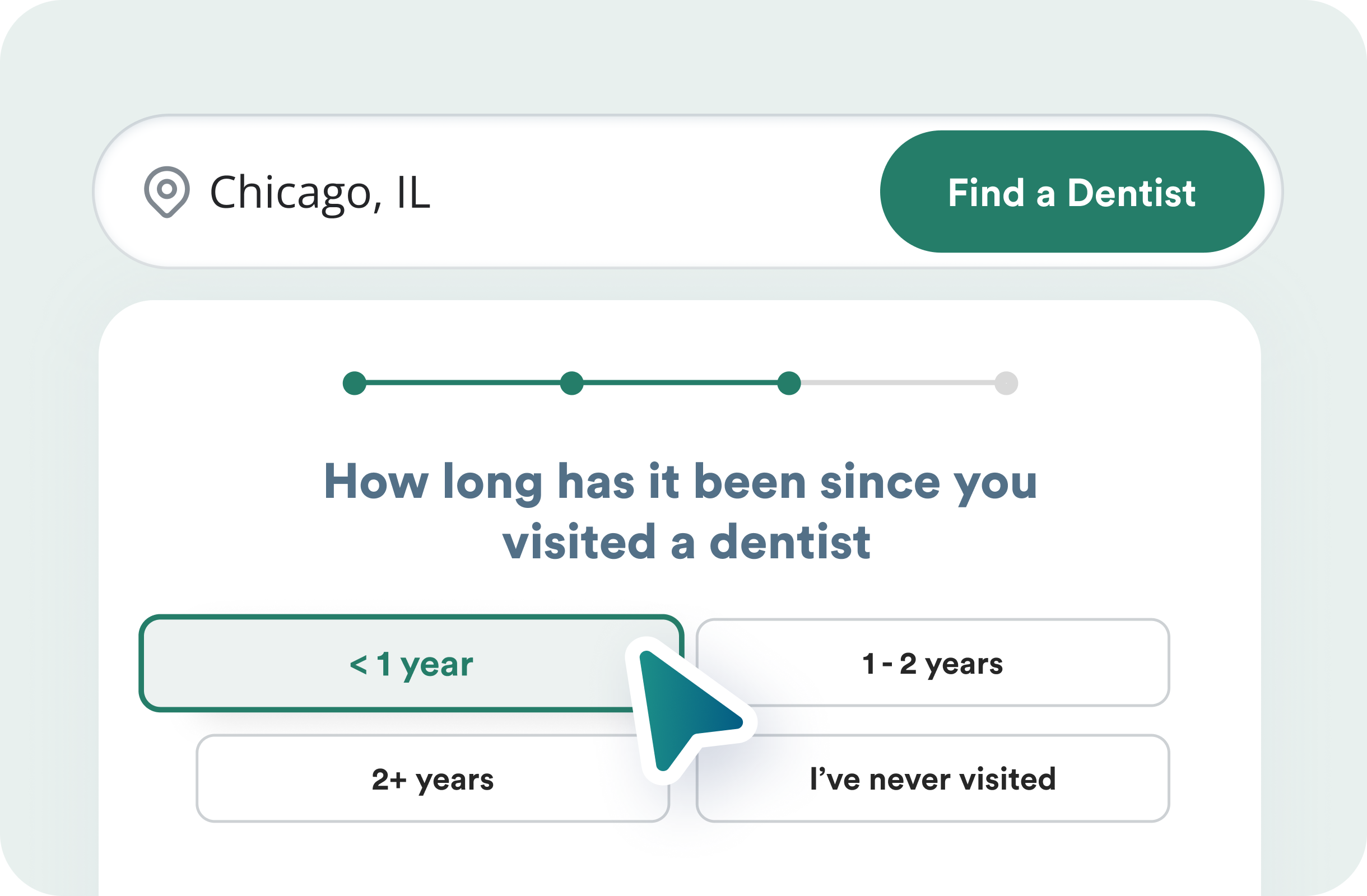
You receive appointment requests in your inbox
Confirm the time they’ve requested or request more insurance info via our built-in SMS chat.

Only pay for successful patient visits
Unlike other marketing options, we only charge you after a successful patient visit. No lead fees for ghost patients.

1 hour to set up & no contracts
We can set you up and integrate with your existing workflows in 1 hour, and you can pause or cancel anytime.
Opencare for DSOs: scalable ROI, minimal lift
Join our network of top dentists today
Frequently asked questions
How does Opencare work?
1 - Our marketing experts find ready-to-book patients: They share their treatment needs, insurance, and preferences – so we can match them with the best dentist for long-term fit.
2 - You receive appointment requests in your inbox: Confirm the time they’ve requested or get more information via our built-in SMS chat.
3 - Only pay for successful patient visits: Unlike other marketing options, we don’t charge you for patients that don’t show up.
4 - 1 hour to set up & no contracts: We set you up and integrate with your existing workflows in 1 hour, and you can pause or cancel your membership anytime.
How do patients find Opencare?
We do all the work! We target thousands of patients everyday across multiple marketing channels including social media, digital advertising, search engines, and our referral network. We’ve perfected patient acquisition so you only have to worry about delivering exceptional care.
Is Opencare operating in my area?
Opencare is available in multiple metropolitan areas across North America and we are quickly expanding our service into new cities every month. Contact us to learn if we are operating in your area.
Does my practice qualify to join the program?
Opencare works exclusively with dentists focused on delivering great patient experiences. In order to qualify, your practice must have a track record of positive reviews online and it must provide patients with a welcoming & safe environment. Opencare does not accept dentists with a history of malpractice.
How fast can I get started on Opencare?
Opencare reviews dentist applications within 2 business days. Once your practice has been approved to join, we will contact your office to schedule a meeting with our team. After a brief orientation and profile setup, your practice will ready to receive its first patient on Opencare!
How much does Opencare cost?
Our pricing model is simple: dentists only pay for new patients that receive dental care. Practice pricing depends on a few factors, including your practice location and your participation in insurance networks. Contact us to get a personalized quote for your practice.
How is Opencare different?
Our philosophy is to deliver value to your practice. Unlike other marketing services and solutions, integrated practices have access to ROI data providing full visibility on earnings. There are no time commitments and no hidden fees - you only pay for results.
.png)